Valentina Guerrini, Ph.D.
Assistant Professor of Medicine
vg238@njms.rutgers.edu
+1-973-854-3212
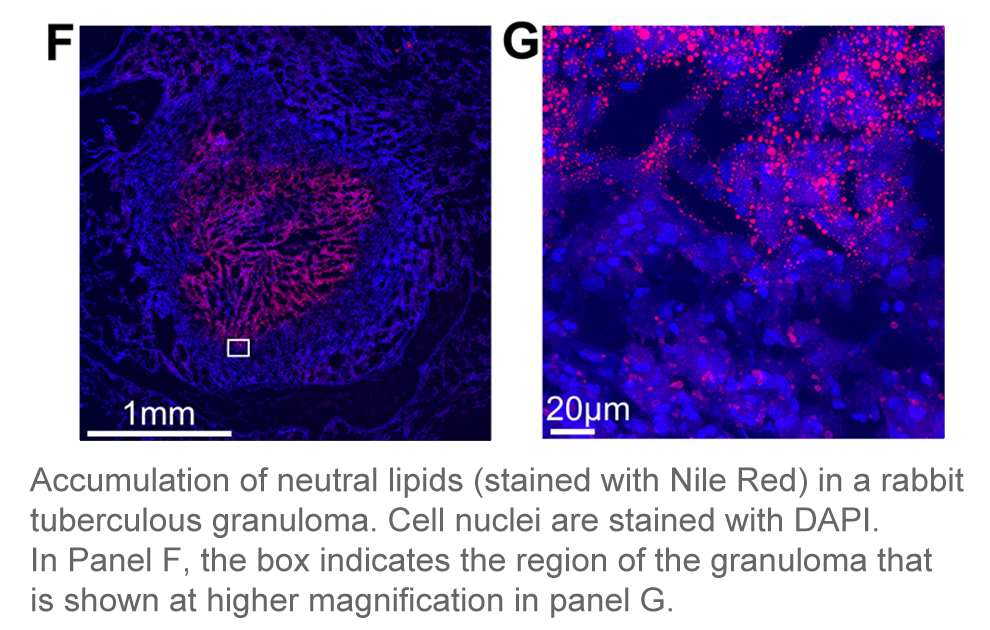
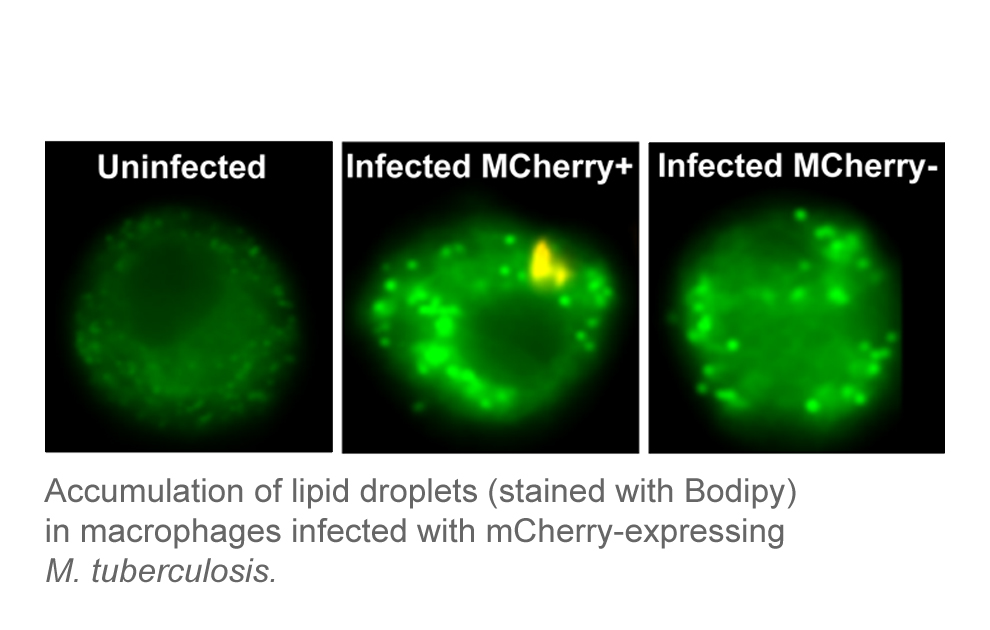
My research focuses on different aspects of innate immune responses to infectious diseases. One aspect that I’m investigating is the link between metabolism and function of innate immune cells. Specifically, my work is focused on lipid metabolism dysregulation in macrophages. Foam cells, lipid-laden macrophages with altered functions, are found in many chronic inflammatory disorders. They are central to tuberculosis pathogenesis and contribute to the pathogenesis of other infectious and non-infectious diseases. My work explores how foam cells generate and contribute to pathogenesis in different immunopathological contexts with the goal of discovering molecular targets for therapeutic intervention or biomarker of disease. Elucidating disease-specific mechanisms of foam cell biogenesis can lead to the efficient targeting of these dysfunctional cells in all diseases they manifest.
The second aspect of innate immunity I’m exploring is sex-bias in immune responses to tuberculosis and other infectious diseases. The main goal of this project is to test the effects of chromosomal and hormonal sex monocyte/macrophage responses to infectious stimuli and determine the molecular mechanisms underlying macrophage sex bias. Identifying the antimycobacterial mechanisms that differ between “female” and “male” macrophages will lead to identifying those that effectively control intracellular infection. We can leverage sexual dimorphism in immune responses to identify the protective ones. Moreover, identifying the biological basis of sex-associated differences in the susceptibility to tuberculosis will have translational implications that are generalizable to other diseases.
My research interests extend also to lung disease caused by non-tuberculous mycobacteria (NTM). Incidence of NTM lung disease is increasing worldwide. One of the major challenges in the clinical management of NTM infections of the lungs is assessing progression of disease or response to treatment. Monitoring treatment response has a particular significance for NTM disease given the complexity of treatment and the frequency of drug-related adverse events. Current approaches in clinical practice have important limitations and an entirely new paradigm is required to improve our approach towards monitoring the course of the treatment for NTM lung disease. My research is focused on the study of the inflammatory environment of the lung, where the infection takes place. The goal is to identify biomarkers of disease by monitoring temporal changes in local immune responses to non-tuberculous mycobacteria. Implementation of biomarkers of disease progression and treatment response in clinical practice would guide clinical decisions and improve management of NTM lung disease.
A complete list of my published work can be viewed in NCBI’s Bibliography at www.ncbi.nlm.nih.gov